Peripheral Neuropathy Feet: Understanding and Managing Foot Pain in Diabetes
Peripheral neuropathy, especially in the feet, is a significant complication of diabetes. It is characterized by nerve damage, which causes pain, numbness, and a range of other symptoms that can severely affect quality of life.
10/13/20247 min read
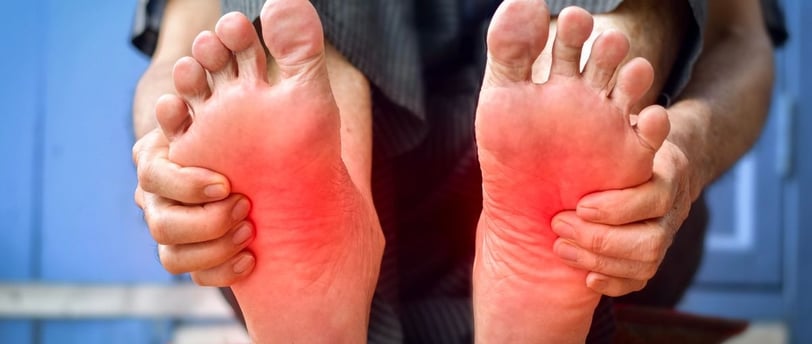
Peripheral Neuropathy Feet: Understanding and Managing Foot Pain in Diabetes
Peripheral neuropathy, especially in the feet, is a significant complication of diabetes.
It is characterized by nerve damage, which causes pain, numbness, and a range of other symptoms that can severely affect quality of life.
Managing this condition is essential to avoid further complications, including foot ulcers, infections, and even amputation.
In this comprehensive guide, we will explore the causes, symptoms, complications, and management strategies for peripheral neuropathy in feet, focusing on key topics such as diabetic feet, foot ulcers, and the prevention of diabetic sores.
What is Peripheral Neuropathy in Feet?
Peripheral neuropathy is a condition caused by long-term high blood sugar levels, leading to nerve damage, particularly in the extremities like the feet.
It's one of the most common complications of diabetes and is a leading cause of diabetic foot pain. Around 60-70% of individuals with diabetes develop some form of neuropathy, and the feet are often the first area to be affected.
This condition, known as neuropathy in feet, can range from mild tingling sensations to intense pain, and in severe cases, it can lead to numbness that increases the risk of unnoticed injuries and infections.
Key Symptoms of Peripheral Neuropathy in Feet:
Tingling and Burning: Many individuals with peripheral neuropathy report a constant tingling or burning sensation, especially at night.
Numbness: As the nerve damage progresses, individuals may experience numbness, making it difficult to feel injuries, like cuts or diabetic sores.
Sharp Pain: Sudden, sharp pain triggered by light touch or pressure can be common in those with diabetic neuropathy.
Increased Sensitivity: Even light contact, such as wearing socks or shoes, can cause discomfort. In some cases, this makes it difficult to walk or carry out everyday activities.
Why are Diabetic Feet Vulnerable?
The feet are particularly vulnerable to complications in individuals with diabetes due to a combination of nerve damage and reduced blood flow.
Peripheral neuropathy foot diabetes occurs because the nerves in the feet are far from the heart, making them more susceptible to damage caused by high blood sugar levels.
When blood sugar remains uncontrolled, the nerves lose their ability to properly communicate with the brain, leading to the symptoms associated with neuropathy in feet.
Reduced Blood Flow in Diabetic Feet:
In addition to nerve damage, individuals with diabetes often experience reduced circulation, particularly in the legs and feet.
This reduced blood flow can starve the feet of oxygen and essential nutrients, slowing the healing process for injuries.
This makes people with diabetes more prone to developing complications such as foot ulcers, diabetic sores, and infections.
Without adequate blood flow, even minor injuries like blisters or cuts can turn into diabetic ulcers. These ulcers, if not properly treated, can become infected and lead to serious complications, such as gangrene or amputation.
For this reason, understanding how diabetes and feet are connected is critical to avoiding long-term damage.
Complications of Peripheral Neuropathy in Feet
Without proper care and management, peripheral neuropathy feet can lead to serious complications, many of which are life-threatening.
One of the most significant dangers is the development of foot ulcers and infections, which are difficult to treat and can lead to amputation if left unchecked.
Foot Ulcers in Diabetic Feet:
One of the most common complications of neuropathy in feet is the development of foot ulcers.
These open sores typically form on pressure points, such as the heel or the ball of the foot, and can result from poorly fitting shoes, friction, or unrecognized injuries.
Because many individuals with feet with neuropathy have diminished sensation, these ulcers may go unnoticed until they become severe.
Once an ulcer develops, it can easily become infected, especially if proper wound care is not administered.
Infections can spread quickly, and in severe cases, they may necessitate amputation of the affected area to prevent the infection from spreading further.
This is why regular foot inspections and early intervention are key to preventing diabetic foot ulcers from progressing to more dangerous stages.
Diabetic Sores on Feet:
Individuals with diabetes are more prone to developing sores on their feet due to a combination of nerve damage and poor circulation.
Diabetic sores can form from even minor injuries, such as a small cut or blister. These sores are often slow to heal due to reduced blood flow and can become infected if not properly treated.
Common locations for these sores include the toes, sides of the feet, and heels.
Diabetic ulcer on toe is one of the more serious conditions that can develop, and it requires immediate medical attention to avoid infection.
Amputation Risks:
When diabetic ulcers and infections are left untreated, amputation may be necessary to prevent the spread of infection. In the United States, diabetes is responsible for approximately 70,000 lower-limb amputations each year.
Most of these cases result from severe diabetic sores on feet or foot ulcers that could not be controlled. Preventing these outcomes requires early detection and effective treatment of any foot injuries or sores.
Managing Peripheral Neuropathy in Feet
While peripheral neuropathy feet can be challenging to manage, there are steps you can take to reduce pain and prevent complications.
Proper foot care, combined with medical treatments and lifestyle changes, can help mitigate the effects of neuropathy in feet and improve overall foot health.
Foot Care Tips:
Daily Inspections: Regular foot inspections are essential for detecting injuries early. Check your feet daily for signs of cuts, blisters, or other abnormalities.
Use a mirror to check the soles of your feet, or ask a family member for help.
Proper Footwear: Always wear shoes that fit well and provide good support.
Avoid wearing shoes that are too tight or cause friction, as this can lead to blisters and foot ulcers. Consider using orthotic shoes or inserts if necessary.
Moisturize Regularly: Keep your feet moisturized to prevent dry, cracked skin, which can lead to diabetic sores.
However, avoid applying lotion between the toes, as excessive moisture can encourage fungal infections.
Medical Treatments for Neuropathy in Feet:
Over-the-Counter Pain Relief: Mild discomfort from neuropathy in feet can be managed with over-the-counter pain relievers like ibuprofen or acetaminophen. These medications can provide temporary relief but do not address the root cause of nerve pain.
Prescription Medications: For more severe pain, your healthcare provider may prescribe medications designed to treat nerve pain. These may include anticonvulsants, antidepressants, or topical treatments that target nerve pain directly.
Physical Therapy: Some individuals benefit from physical therapy treatments, such as Intraneural Facilitation (INF), which helps improve blood flow to the nerves and reduce pain. Regular therapy sessions can also improve mobility and prevent further complications.
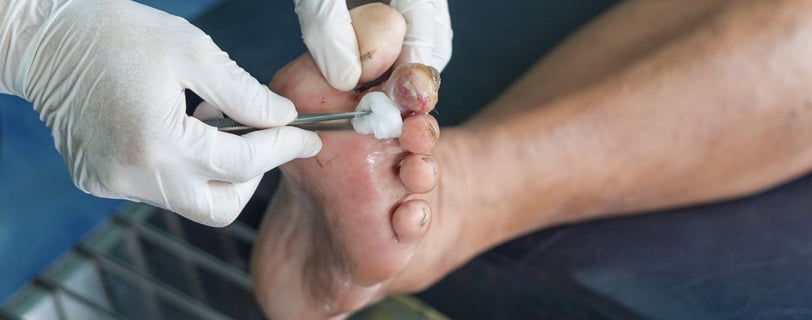
Preventing Diabetic Foot Ulcers and Sores
The best way to avoid serious complications like diabetic ulcers and sores is to take preventative measures.
Managing blood sugar levels, adopting a healthy lifestyle, and following a consistent foot care routine can significantly reduce your risk of developing foot ulcers and other complications related to diabetes and feet.
Blood Sugar Control:
Maintaining target blood glucose levels is essential for preventing further nerve damage and reducing the risk of complications.
Regular monitoring of blood sugar levels, adherence to prescribed medications, and following a balanced diet are crucial steps in managing diabetic feet and preventing neuropathy from worsening.
Exercise for Foot Health:
Regular physical activity can help improve circulation and strengthen the muscles in your legs and feet.
Activities such as walking, swimming, or cycling can increase blood flow to the extremities, helping to maintain healthy nerve function and prevent the development of foot ulcers.
Routine Check-Ups:
Regular visits to your healthcare provider and a podiatrist are vital for keeping diabetic foot pain in check.
During routine exams, your doctor can detect early signs of complications, such as ulcers on feet or diabetic sores, and provide treatment before the condition worsens.
Additional Preventative Measures for Peripheral Neuropathy in Feet
Healthy Habits for Diabetic Foot Care:
Incorporating healthy habits into your daily routine is crucial for managing peripheral neuropathy feet and preventing further complications.
This includes maintaining a balanced diet rich in whole foods, fruits, vegetables, and lean proteins. These nutrient-rich foods help support overall health and blood sugar control, both of which are key factors in preventing diabetic foot complications.
Keeping Feet Protected:
Always protect your feet by wearing socks and shoes, even when indoors. Bare feet are more susceptible to injuries, and for individuals with neuropathy in feet, even a small injury can lead to serious problems.
Consider using padded or diabetic socks that provide extra cushioning and reduce the risk of friction and pressure.
Conclusion
Peripheral neuropathy in feet is a serious complication of diabetes that can lead to significant discomfort and dangerous health risks.
By understanding the causes of neuropathy in feet, recognizing the symptoms, and following a proactive care plan, individuals with diabetes can significantly reduce their risk of developing severe complications such as diabetic foot ulcers, infections, and amputations.
Managing diabetic feet requires a comprehensive approach that includes proper foot care, blood sugar management, and regular medical check-ups.
By staying vigilant and addressing foot issues early, you can prevent the progression of peripheral neuropathy foot diabetes and maintain a better quality of life. Taking care of your feet today ensures long-term health and mobility, allowing you to avoid the most severe
Thank you for taking the time to read this comprehensive guide on managing peripheral neuropathy in feet and understanding the complications associated with diabetes and foot health.
While proactive foot care and lifestyle changes can significantly reduce the risk of foot ulcers and other complications, it’s important to remember that each person’s situation is unique.
Always consult a healthcare professional for personalized advice and treatment options tailored to your specific needs. Managing diabetes and foot health requires ongoing attention, and working closely with your doctor or podiatrist will help ensure the best possible outcomes.
Your feet are essential to your overall well-being, so taking steps today to care for them can help prevent future complications and improve your quality of life. Stay vigilant, seek medical support when needed, and continue prioritizing your health.
Subscribe to our Newsletter
Enjoy exclusive Special Deals Available Only to Our Subscribers.



